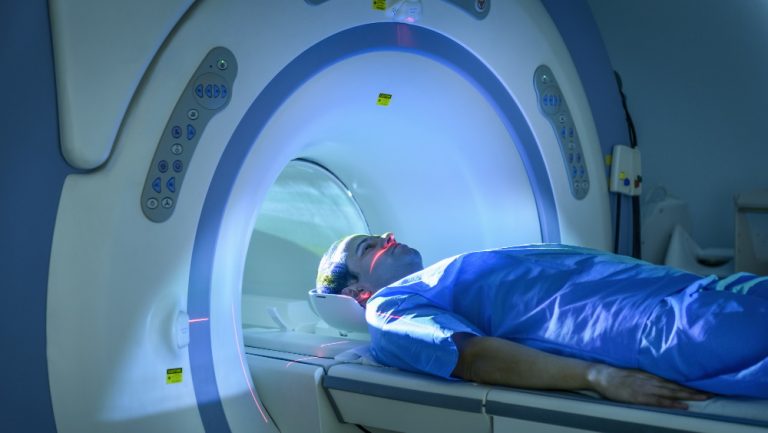
The Role Of Monitoring In Ensuring Efficacy
Monitoring the effectiveness of cancer treatment is crucial for ensuring that patients receive the most appropriate and personalized care. By tracking patients’ progress closely, healthcare providers can detect issues early and make necessary adjustments to maximize treatment efficacy and minimize side effects.
Regular monitoring assesses tumor response, including size, tumor markers, and patient well-being, guiding decisions about therapy continuation or modification. It also helps identify and manage adverse reactions to improve patient comfort and quality of life.
Monitoring provides valuable data for medical research, contributing to the development of innovative therapies and a deeper understanding of cancer. This data can guide future advancements in cancer care and identify potential areas for further research.
Standard Monitoring Techniques In Cancer Treatment
There are several techniques and tools that healthcare professionals use to monitor cancer treatment and assess its efficacy. These methods vary depending on the type and stage of cancer and the specific treatment approach. Some of the standard monitoring techniques include:
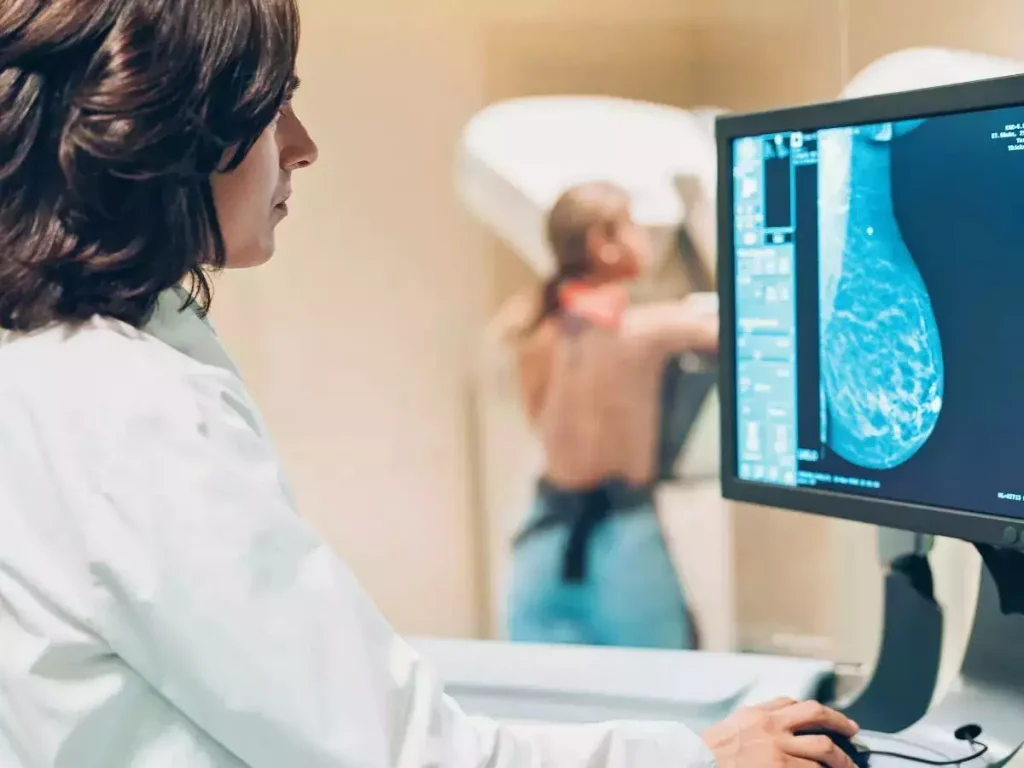
- Imaging: Imaging techniques such as computed tomography (CT), magnetic resonance imaging (MRI), and positron emission tomography (PET) scans are widely used to visualize tumors and monitor their response to treatment. According to a radiology specialist at Kimball Health Services, these imaging modalities provide detailed information about tumor size, location, and changes over time, allowing healthcare professionals to assess treatment effectiveness.
- Laboratory tests: Laboratory tests, including blood tests and tumor marker assessments, are crucial in monitoring cancer treatment. These tests help measure specific substances or biomarkers that indicate the presence or progression of cancer. By regularly monitoring these markers, healthcare professionals can track treatment responses and make necessary adjustments.
- Physical examinations: Regular physical examinations are essential for monitoring cancer treatment. These examinations assess vital signs, physical appearance, and overall patient well-being. By examining the patient and reviewing their symptoms, healthcare professionals can identify any changes or complications requiring further investigation or intervention.
- Patient-reported outcomes: Patient-reported outcomes (PROs) are essential to monitoring cancer treatment. These outcomes include patient-reported symptoms, quality-of-life assessments, and self-reported experiences with treatment. By actively involving patients in reporting their experiences, healthcare providers can gain valuable insights into treatment efficacy and tailor interventions to meet individual needs.
Benefits Of Regular Monitoring During Cancer Treatment
Regular monitoring during cancer treatment offers many benefits, including early detection of treatment failure, minimizing side effects, personalized care, and contributing to medical research. By identifying signs of treatment failure early, healthcare providers can adjust plans promptly for better outcomes. Monitoring also helps manage side effects, improving patient comfort and well-being. Personalized treatment adjustments based on response and quality of life assessments enhance overall care. Additionally, monitoring provides valuable data for medical research, informing the development of new therapies and advancements in cancer care.
Challenges And Limitations Of Monitoring Cancer Treatment
Monitoring cancer treatment has significant benefits but also faces challenges and limitations. These include variability in individual response, resource availability, patient compliance, and data interpretation. Differences in treatment responses require flexible monitoring approaches for accurate efficacy assessment. Limited access to resources such as imaging facilities and specialized healthcare can impact monitoring frequency and accuracy. Patient compliance is essential, as understanding and engaging in the process influences monitoring effectiveness. Interpreting monitoring data demands expertise to analyze results accurately for informed treatment decisions.
The Importance Of Personalized Monitoring Plans
To maximize the effectiveness of cancer treatment monitoring, personalized monitoring plans are essential. Each patient’s monitoring plan should be tailored to their cancer type, treatment approach, and individual needs. Personalized monitoring plans consider factors such as the cancer stage, treatment goals, potential side effects, and the patient’s overall health.
By customizing monitoring plans, healthcare providers can ensure that patients receive the most appropriate care and that treatment efficacy is accurately assessed. Personalized plans may include specific imaging schedules, laboratory tests, and symptom assessments relevant to the patient. Regular communication between healthcare providers and patients is crucial to ensure that monitoring plans are followed and any concerns or changes are promptly addressed.
Technology Advancements In Cancer Treatment Monitoring
Advancements in technology have significantly enhanced the monitoring of cancer treatment. These advancements have improved the accuracy, efficiency, and accessibility of monitoring techniques. Some notable technological advancements include:
- Artificial intelligence (AI): AI algorithms can analyze large volumes of imaging data and assist healthcare professionals in detecting subtle changes or patterns that may indicate treatment response or disease progression.
- Telemedicine: Telemedicine platforms enable remote monitoring and communication between healthcare providers and patients. This technology allows patients to report symptoms, participate in virtual consultations, and share monitoring data without the need for frequent hospital visits.
- Mobile applications: Mobile applications designed for cancer patients can help monitor symptoms, track medication adherence, and provide educational resources. These apps facilitate patient engagement and enable healthcare providers to monitor patient progress remotely.
- Wearable devices: Wearable devices, such as smartwatches and fitness trackers, can collect real-time data on physical activity, heart rate, sleep patterns, and other relevant metrics.
In addition to these advancements, incorporating the OncoCount test by RGCC-North America into personalized monitoring plans enhances the comprehensive assessment of treatment response. The OncoCount test measures circulating tumor cells (CTCs) in the bloodstream, providing valuable insights into treatment effectiveness and disease progression. By regularly monitoring CTC counts, healthcare providers can promptly identify changes indicative of treatment response or recurrence, allowing for timely adjustments to the treatment approach. Integrating OncoCount into personalized monitoring plans ensures a more thorough and tailored approach to cancer treatment monitoring, ultimately improving patient outcomes and quality of life.
Conclusion: The Future Of Cancer Treatment Monitoring
In conclusion, monitoring cancer treatment is critical to delivering effective care. By closely tracking progress and making timely adjustments, healthcare providers can significantly improve treatment outcomes, enhance patient well-being, and contribute to ongoing medical advancements in the fight against cancer.
The future of cancer treatment monitoring holds great promise. Advancements in technology, such as AI and telemedicine, will continue to improve the accuracy and accessibility of monitoring techniques. Personalized monitoring plans will become more sophisticated, considering individual patient characteristics and treatment goals.